Scientific evidence for cold water immersion and stress tolerance
Introduction to Cold Exposure and Stress Habituation
The intentional application of cold water for therapeutic purposes has historical precedents dating back millennia, but modern cold water immersion (CWI) and cold shower protocols have recently gained substantial traction as interventions for physical recovery, stress resilience, and psychological well-being. Proponents often assert that brief, deliberate exposure to cold environments functions as an adaptogen - a stimulus that trains the central and autonomic nervous systems to handle physiological and psychological stressors more effectively.
However, the rapid popularization of cold therapy has outpaced rigorous clinical validation, leading to a conflation of subjective wellness trends with objective physiological data. A central debate in contemporary research is whether the psychological benefits reported by practitioners - such as elevated mood, increased focus, and reduced anxiety - are the result of a genuine adaptogenic effect driven by neurochemical and autonomic adaptations, or whether they are primarily driven by expectancy, mindset, and the placebo effect.
Research indicates that cold water exposure elicits profound physiological responses, including massive catecholamine surges, systemic vasoconstriction, and delayed parasympathetic rebound 121. Yet, when translating these acute physiological markers into long-term psychological outcomes, the data reveals significant methodological limitations, including small sample sizes, lack of active control groups, and inherent difficulties in blinding participants to temperature interventions 2. The scientific consensus suggests a complex interplay: the physiological shock is undeniable and provides measurable autonomic conditioning, but the translation of this shock into sustained mental health benefits is highly variable and heavily influenced by cognitive framing.
Autonomic and Endocrine Mechanisms of Cold Habituation
The immediate physiological reaction to sudden cold exposure is termed the "cold shock response." This response is characterized by a rapid, involuntary gasp, hyperventilation, peripheral vasoconstriction, and a severe spike in heart rate and blood pressure 15. The body's primary objective during this phase is to defend core temperature and preserve homeostasis by redirecting warm blood from the extremities to vital organs 37.
The Cold Shock Response and Sympathetic Activation
The initial phase of CWI is dominated by the sympathetic nervous system. Cutaneous thermoreceptors rapidly transmit signals to the hypothalamus, triggering a systemic cascade. Research measuring neurochemical responses to full-body immersion in 14°C water has documented a 530% increase in plasma norepinephrine (noradrenaline) and a 250% increase in dopamine 128. Norepinephrine plays a crucial role in attention, arousal, and mood regulation, while dopamine is associated with motivation and reward pathways.
While these figures are frequently cited as evidence for the profound cognitive benefits of cold plunging, neurophysiological experts urge calibrated interpretation. A critical distinction must be made between peripheral and central neurotransmitter levels. Increased dopamine in the peripheral nervous system, which circulates throughout the body, does not necessarily cross the blood-brain barrier to produce the central nervous system effects often claimed in mainstream wellness discourse 4. Peripheral dopamine is primarily involved in localized vascular and renal functions 4.
Furthermore, the adaptation to these catecholamine spikes changes with chronic exposure. A 2025 study evaluating regular winter swimmers found that while they possessed higher baseline adrenaline levels than a control group (225.6 pmol/L versus 153.8 pmol/L), a single bout of cold water immersion resulted in a significant reduction in noradrenaline and adrenaline concentrations 24 hours post-immersion 5. This suggests a complex, adaptive down-regulation of catecholamines over time rather than a perpetual spike 25.
Parasympathetic Reactivation and Vagal Tone
Following the initial sympathetic surge, habituated practitioners experience a rebound in parasympathetic nervous system activity, often described as a state of calm alertness. This shift is heavily mediated by the vagus nerve, which runs along the neck and responds powerfully to cold stimulation 111.
The parasympathetic response is particularly amplified by the mammalian diving reflex. When the face, specifically the distribution of the trigeminal nerve, is submerged in cold water, it triggers an evolutionary adaptation designed to conserve oxygen. This reflex directly stimulates the vagus nerve, resulting in bradycardia (slowing of the heart rate) and increased parasympathetic dominance 67.
Meta-analytical data confirms that CWI significantly enhances heart rate variability (HRV) indices up to 15 minutes following exposure. Specifically, researchers observed increased Root Mean Square of Successive Differences (RMSSD) and High-Frequency (HF) bands - both markers of parasympathetic activity - alongside a decreased Low-Frequency to High-Frequency (LF/HF) ratio and decreased overall heart rate 8. While cold showers can trigger partial parasympathetic activation, full immersion that covers the neck and chest provides a much more comprehensive vagal stimulus, maximizing cardiac-vagal activation 19.
HPA Axis Response and Cortisol Regulation
The hypothalamic-pituitary-adrenal (HPA) axis governs the body's long-term stress response, culminating in the release of cortisol. Cold exposure reliably triggers acute cortisol secretion as part of the initial stress response 110. However, the therapeutic hypothesis behind CWI is that repeated, controlled activation of the HPA axis leads to habituation.
Research indicates that individuals who repeatedly expose themselves to cold water exhibit blunted cortisol reactivity not only to the cold itself but also to subsequent, unrelated stressors 610. In specific trials measuring cortisol, serum levels normalized faster in habituated practitioners, though exact baseline shifts remain inconsistent across study populations 11. This reduced cortisol response implies enhanced systemic resilience, suggesting that the body's threshold for perceiving stimuli as threatening has been raised over successive exposures.
Psychological Outcomes and the Placebo Effect
A pervasive claim in commercial wellness is that cold plunging significantly mitigates anxiety and depression. The scientific reality is vastly more nuanced. While physiological responses to cold are robust, isolating the psychological outcomes from the placebo effect remains a significant methodological challenge in hydrotherapy research.
Cross-Stressor Habituation Theory
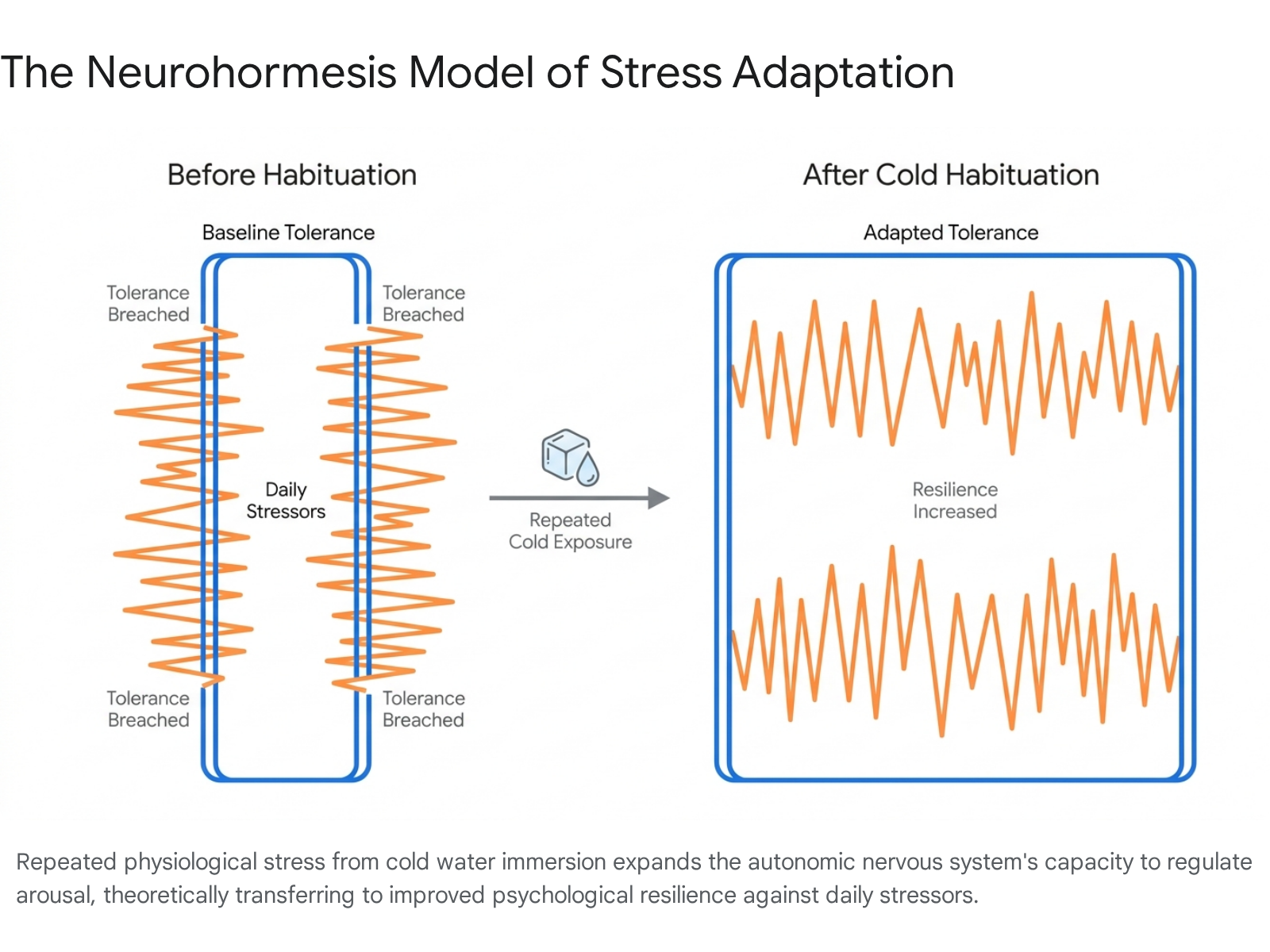
The concept of "cross-stressor habituation" or "neurohormesis" forms the biological rationale for CWI's psychological benefits. Neurohormesis posits that exposure to a mild, controlled physical stressor fortifies neural pathways, enhancing the central nervous system's capacity to tolerate other forms of psychosocial stress 210.
By repeatedly subjecting the body to the severe discomfort of freezing water and forcing the autonomic nervous system to regulate respiration and heart rate, practitioners train top-down cognitive control over involuntary physiological panic. This repeated physiological habituation is believed to transfer to psychological resilience, enabling better emotional regulation during daily psychosocial stressors 110.
Functional MRI studies support this, demonstrating that a single bout of cold water immersion increases connectivity between large-scale brain networks involved in emotional regulation, including the prefrontal cortex and anterior insula 8.
Meta-Analytical Data on Mood and Anxiety
A comprehensive 2025 systematic review and meta-analysis published in PLOS One (comprising 11 randomized controlled trials and 3,177 participants) rigorously evaluated the psychological and physiological effects of CWI in healthy adults. The analysis tracked both immediate and delayed markers across multiple timepoints.
Data indicates a notable temporal disconnect between acute physiological markers and subjective psychological relief. While plasma norepinephrine peaks acutely during the immersion itself, subjective perceived stress levels show statistically significant reductions at a delayed 12-hour interval.
| Measurement Domain | Marker / Instrument | Acute Post-Exposure Effect | 12-Hour Post-Exposure Effect | 24-Hour Post-Exposure Effect |
|---|---|---|---|---|
| Endocrine / Autonomic | Norepinephrine | Spike (up to 530% of baseline) 28 | Gradual return to baseline | Return to baseline / Slight reduction 5 |
| Inflammation | Cytokine Release | Significant Increase (SMD: 1.03) 1 | Normalizing | Return to baseline 1 |
| Psychological Stress | Perceived Stress Scale | No significant change (SMD: -0.09) 1 | Significant Reduction (SMD: -1.00) 1 | No significant change (SMD: -0.06) 1 |
Regarding mood, depression, and anxiety, the meta-analytical data is highly mixed. While some small-scale studies report immediate mood elevation and increased positive affect following brief immersions in ~20°C water 618, the 2025 PLOS One meta-analysis found no consistent, statistically significant differences in long-term mood across the broader data pool 1. Much of the evidence supporting CWI for clinical depression or anxiety relies on small sample sizes, lacks active control groups, and utilizes non-clinical, healthy volunteer populations 212.
The Influence of Mindset and Expectancy
The placebo effect and psychological expectancy are impossible to fully blind in cold water trials; participants are acutely aware of whether they are in ice water or a lukewarm control bath. Dr. Mark Harper, a prominent researcher in cold-water swimming, acknowledges that the reported mood enhancements may be heavily influenced by placebo 1314. The psychological triumph of overcoming a deeply aversive stimulus yields an immediate boost in self-efficacy and self-esteem. As Harper notes, the mindset of "I have accomplished this difficult task; therefore, I can accomplish anything" is a potent, non-pharmacological mood elevator independent of thermoregulation 13.
Furthermore, mindset fundamentally alters physiological responses. A 2025 Stanford University study demonstrated that a brief intervention designed to shift participants' mindsets about catastrophic stress resulted in lower levels of depression and reduced C-reactive protein (an inflammatory marker) months later 15. Similarly, in cold exposure research, individuals with higher baseline optimism and positive expectancy regarding the intervention demonstrate higher levels of epinephrine and greater concentrations of the anti-inflammatory cytokine interleukin-10 (IL-10) during exposure 11. Therefore, the belief in the efficacy of the cold plunge biologically potentiates its benefits, blurring the line between pure physiological adaptation and psychoneuroimmunological response.
Efficacy of Modalities: Showers Versus Full Immersion
The debate between cold showers and full-body cold water immersion centers on accessibility versus physiological depth. While cold showers are highly accessible and require no specialized equipment, they deliver a fundamentally different stimulus than full submersion in an ice bath.
Hydrostatic Pressure and Thermal Gradients
In an ice bath, the entire body up to the neck is submerged in uniformly cold water. Water conducts heat away from the body roughly 24 times faster than air, and full immersion ensures that the entire skin surface area is simultaneously subjected to a severe thermal gradient. Furthermore, full immersion subjects the body to hydrostatic pressure - the inward force exerted by the water. Hydrostatic pressure actively assists in venous return, pushing blood from the extremities back toward the heart, which aids in the clearance of metabolic waste and reduces edema in damaged muscle tissue 2324.
Conversely, a cold shower provides intermittent cooling. Water flows over specific parts of the body while other areas remain exposed to ambient air. Because the cardiovascular and neurochemical response to cold is directly proportional to the surface area exposed and the speed of heat loss, cold showers produce a significantly blunted autonomic response. They lack hydrostatic pressure and do not cool deep muscle tissue rapidly enough to match the anti-inflammatory and athletic recovery benefits of full immersion 123.
Sickness Absence and Immune Modulation
Despite their physiological limitations compared to ice baths, cold showers exhibit measurable health benefits, particularly regarding immune function and resilience to minor pathogens. The landmark 2016 "Cool Challenge" study conducted in the Netherlands randomized 3,018 adults to end their daily warm shower with 30, 60, or 90 seconds of cold water for 30 consecutive days 16.
The results, analyzed via a negative binomial regression model, demonstrated a 29% reduction in self-reported sickness absence from work among the cold shower groups compared to the control group (Incident Rate Ratio: 0.71, P = 0.003) 1617. Notably, there was no significant difference in the total number of illness days reported; participants still contracted mild illnesses at similar rates, but their symptom severity was modulated to a degree that allowed them to continue functioning and attend work 161718.
Interestingly, the duration of the cold shower (30 vs. 60 vs. 90 seconds) did not change the outcome, suggesting that the initial 30-second cold shock is sufficient to trigger the immune-modulating response 2319.
| Feature / Outcome | Cold Shower (Partial Exposure) | Cold Water Immersion (Full Submersion) |
|---|---|---|
| Thermoregulation | Intermittent cooling; slow core temperature drop. | Uniform cooling; rapid, continuous heat extraction. |
| Vagal Stimulation | Weak to moderate; limited neck/face submersion. | Strong; full coverage of the vagus nerve pathways 1. |
| Hydrostatic Pressure | None. Relies purely on temperature for vasoconstriction. | High. Actively forces venous return and clears metabolic waste 23. |
| Neurochemical Release | Mild to moderate increase in alertness and norepinephrine. | Intense spike in norepinephrine (up to 530%) and dopamine 12. |
| Sickness Absence | Proven 29% reduction in work absence 1618. | Assumed similar or greater, though large-scale pragmatic RCTs are lacking. |
| Muscle Recovery | Ineffective for deep tissue cooling and soreness reduction. | Gold standard for reducing DOMS and clearing creatine kinase 120. |
Dose-Response Relationships and Optimal Protocols
Optimizing the dosage of cold water immersion requires balancing the stimulus required to force an adaptation against the risk of systemic overload and hypothermia. The "dose" of cold therapy is determined by a matrix of temperature, duration, and frequency.
Temperature and Duration Parameters
A 2025 network meta-analysis comprising 55 randomized controlled trials evaluated the specific impacts of varying CWI protocols on exercise-induced muscle damage, delayed onset muscle soreness (DOMS), and biochemical markers like creatine kinase (CK) 2021. The data indicates that time and temperature are inversely related: colder water requires less time to achieve the same physiological load 22.
The meta-analysis established the following optimal protocols: * For Neuromuscular Recovery and Biochemical Markers: Medium-Duration, Low-Temperature CWI (10 - 15 minutes at 5°C - 10°C) was the most effective protocol for clearing creatine kinase and restoring explosive power, such as jump performance 2023. * For Perceived Muscle Soreness (DOMS): Medium-Duration, Medium-Temperature CWI (10 - 15 minutes at 11°C - 15°C) proved to the most effective intervention for subjective pain reduction 2023.
Temperatures below 5°C offer rapidly diminishing returns. While extreme cold (1°C - 4°C) triggers an immediate, violent cold shock response that may train mental fortitude, extending exposure beyond a few minutes at these temperatures significantly increases cardiovascular strain and the risk of non-freezing cold injuries without proportionally increasing recovery or metabolic benefits 2233. Furthermore, acute inflammation increases immediately following cold exposure before resolving, indicating that the intervention operates via hormetic stress 1.
Cumulative Weekly Volume and Minimum Effective Dose
Individual session length is less critical than cumulative weekly volume. Research tracking regular winter swimmers identified a threshold for metabolic adaptation. A minimum effective dose of approximately 11 minutes of full-body cold exposure per week - divided across two to three sessions - is sufficient to activate brown adipose tissue, improve insulin sensitivity, and deliver sustained neurochemical benefits 32224.
Beyond this weekly volume, the central nervous system habituates. The stress response diminishes over time, and while cognitive clarity and mood benefits persist, the acute neurochemical spikes (particularly noradrenaline) begin to blunt, preventing chronic stress overload 2.
Demographic Variables in Thermoregulation
The vast majority of early hydrotherapy research was conducted on fit, young men. However, recent systematic reviews highlight that biological sex, body composition, and age drastically alter thermoregulatory responses, necessitating individualized protocols rather than blanket prescriptions.
Biological Sex and Body Composition
Men and women exhibit distinctly different thermoregulatory strategies when subjected to cold water. Women generally possess a higher percentage of body fat, which serves as natural insulation, yet they have a smaller overall volume-to-mass ratio and less skeletal muscle mass 2526. Consequently, women experience faster heat loss from the skin surface.
To defend their core temperature, the female autonomic nervous system initiates aggressive peripheral vasoconstriction earlier than males, shutting off blood flow to the extremities to keep warm blood centralized 332537. Due to this rapid vasoconstriction and smaller muscle mass available for heat generation, women typically reach the threshold for muscle shivering significantly earlier than men 3325. Autonomic load is also influenced by the menstrual cycle; women exhibit more substantial autonomic strain under initial cold stress during the luteal phase, when baseline core temperature is naturally higher 33.
Despite these differences in perception and extremity cooling, studies controlling for body fat percentage and surface area-to-mass ratios reveal that the actual rate of core cooling is not significantly different between sexes during moderate immersion 2728. However, the subjective experience of cold is generally more intense for women. As a result, tailored protocols often suggest women may achieve optimal autonomic adaptations using shorter exposure durations (e.g., 2 - 5 minutes) at slightly warmer temperatures compared to men 333729.
Age-Related Vulnerabilities and Cognitive Benefits
Aging naturally degrades thermoregulatory efficiency. Older adults generally exhibit a delayed vasoconstrictor response, reduced muscle mass for shivering thermogenesis, and impaired thermal perception, making them more vulnerable to hypothermia and excessive cardiovascular strain during environmental cold exposure 3031. The sharp spike in blood pressure during the cold shock response presents a non-trivial risk for older individuals with underlying cardiovascular conditions 32.
Conversely, carefully controlled CWI combined with mindfulness interventions has shown unique benefits for aging populations when safety parameters are observed. A 2025 pilot study examining a combined mindfulness and CWI program over 20 weeks found a significant reduction in depressive symptoms (mean difference = -2.59, p = 0.003), with the intervention demonstrating higher effectiveness for older adults compared to middle-aged participants 3334. This indicates that while physiological risks increase with age, the psychological and neurohormetic benefits of cold therapy remain highly relevant for older demographics.
Synergistic Interventions and Breathwork Methodologies
The intersection of cold exposure with conscious breathwork has been popularized largely by the Wim Hof Method (WHM), which combines voluntary hyperventilation, breath retention, cold therapy, and psychological commitment 1135. The primary claim of WHM is that the combination of these pillars yields synergistic effects on the immune and autonomic nervous systems that neither practice can achieve alone.
Combined Interventions and Endotoxemia
A 2024 systematic review published in PLOS One analyzed nine trials investigating the WHM. The review concluded that the method holds significant promise in the inflammatory response category. Practitioners successfully elevated epinephrine levels, which in turn increased anti-inflammatory cytokines (such as IL-10) and suppressed pro-inflammatory cytokines (such as TNF-α, IL-6, and IL-8) during experimental endotoxemia (the intravenous administration of E. coli endotoxin) 113536.
Isolation of Components in Factorial Trials
However, the assertion that breathwork and cold exposure are strictly synergistic has recently been challenged. A 2026 factorial randomized controlled trial isolated the components of the WHM, placing participants into four distinct groups: breathwork only, cold exposure only, breathing plus cold, and a control group. Following an endotoxin injection to stimulate an inflammatory response, the researchers found that while both breathing and cold exposure independently reduced inflammation, the combined "breathing plus cold" group did not perform significantly better than either component in isolation 37.
The physiological pathways remain distinct: breathwork primarily drives epinephrine-mediated anti-inflammatory effects, while cold water drives HPA-axis and norepinephrine responses 37. Therefore, while the combination is highly effective, the relationship appears to be additive rather than a synergistic multiplier. The insistence on combining the two may serve primarily to provide practitioners with a psychological focal point - a coping mechanism - during the intense discomfort of the ice bath, rather than unlocking entirely new physiological adaptations 37.
Conclusion
The scientific consensus indicates that cold water immersion exerts a genuine, measurable adaptogenic effect on the human body, extending well beyond a mere psychological placebo. The physiological mechanisms - characterized by massive acute catecholamine surges, profound vagus nerve stimulation via hydrostatic pressure and the diving reflex, and acute modulation of inflammatory cytokines - are rigorously documented across multiple randomized controlled trials. The cross-stressor habituation theory provides a valid biological framework for how repeatedly managing the acute panic of freezing water trains the autonomic nervous system to better regulate arousal during daily psychosocial stressors.
However, claims regarding the psychological outcomes of cold therapy require heavy qualification. The data supporting CWI as a standalone, clinical treatment for depression or anxiety remains weak, often plagued by small sample sizes and the impossibility of blinding participants to the placebo effect of surviving an extreme challenge. Furthermore, the massive increases in dopamine frequently touted in wellness circles represent peripheral circulating dopamine, which does not easily translate to the central nervous system focus and motivation often advertised.
Optimal dosing leans away from extreme suffering and aligns with moderate, consistent exposure: approximately 11 to 15 minutes per week at 10°C to 15°C is sufficient to trigger maximal biochemical recovery, activate parasympathetic rebound, and instigate brown fat adaptation without risking hypothermic overload or excessive cardiovascular strain. Ultimately, while cold water is not a panacea for mental health disorders, it remains a highly potent, evidence-based tool for autonomic regulation, athletic recovery, and the cultivation of physiological resilience.