Longitudinal evidence on rising adolescent anxiety disorders
The epidemiological landscape of adolescent mental health has undergone a pronounced shift over the past two decades, characterized by steep increases in the reported prevalence of anxiety disorders, depressive episodes, and associated behavioral sequelae. While historical data prior to the early 2010s depicted relatively stable baseline rates of youth internalizing disorders, longitudinal population surveys across multiple continents now demonstrate a synchronized upward trajectory. This phenomenon has prompted extensive multidisciplinary inquiry into the structural, technological, and cultural drivers of adolescent psychological distress.
Addressing the etiology of rising adolescent anxiety disorders requires disentangling a complex matrix of causal variables. Current empirical literature points to four primary domains: the neurobiological and behavioral impacts of digital technology and algorithmic social media; the intensification of transnational academic and socioeconomic pressures; the exacerbating effects of the COVID-19 pandemic on an upward-trending baseline; and the epidemiological complexities introduced by "prevalence inflation," wherein widespread mental health awareness campaigns may be inadvertently lowering the threshold for clinical self-identification.
Global Epidemiological Incidence and Prevalence
Analyses of cross-national databases reveal that the escalation of adolescent anxiety is a geographically broad, though not entirely uniform, phenomenon. Understanding the exact contours of this rise requires examining large-scale epidemiological datasets that track diagnostic incidence and prevalence over time.
Shifts in Global Baseline Data
The Global Burden of Disease (GBD) 2021 study provides a comprehensive longitudinal assessment of adolescent anxiety over three decades. Between 1990 and 2021, the global incident cases of anxiety disorders among adolescents and young adults (aged 10 - 24 years) increased by 52.00% 1. The global incidence rate rose from 708.02 per 100,000 in 1990 to 883.10 per 100,000 in 2021 1. Joinpoint regression analyses within the GBD data indicate that this growth was not linear; incidence rates experienced a gradual decline until 2001, followed by a slow, steady increase until 2019, which then culminated in a sharp, statistically significant spike between 2019 and 2021 1.
Prevalence data mirrors these incidence trajectories. The global prevalence rate increased from 4,120.60 per 100,000 in 1990 to 4,976.61 per 100,000 in 2021 1. Disability-Adjusted Life Years (DALYs) due to anxiety disorders in this age cohort similarly increased by 104.85% over the same period, signaling a profound escalation in the functional impairment associated with these conditions 1. Across all global metrics, the data identifies gender as a primary axis of disparity: incidence and prevalence rates of anxiety disorders are consistently higher among adolescent females than males across all geographic and socioeconomic strata 1.
United States Diagnostic Trajectories
Within the United States, diagnostic prevalence data closely tracks the global acceleration. Between 2016 and 2023, the prevalence of diagnosed mental or behavioral health conditions among U.S. adolescents aged 12 - 17 increased by 35%, rising from 15.0% to 20.3% 2. Specifically, the prevalence of diagnosed anxiety within this cohort increased by 61% (rising from 10.0% to 16.1%), making it the most common condition ahead of depression (8.4%) and behavioral or conduct problems (6.3%) 2. Similar to global trends, the 2023 U.S. data indicates that a significantly greater proportion of adolescent females had diagnosed anxiety (20.1%) compared to males (12.3%) 2.
Furthermore, data tracking clinical severity found that rates of emergency department visits for self-harm among U.S. early adolescents accelerated dramatically.
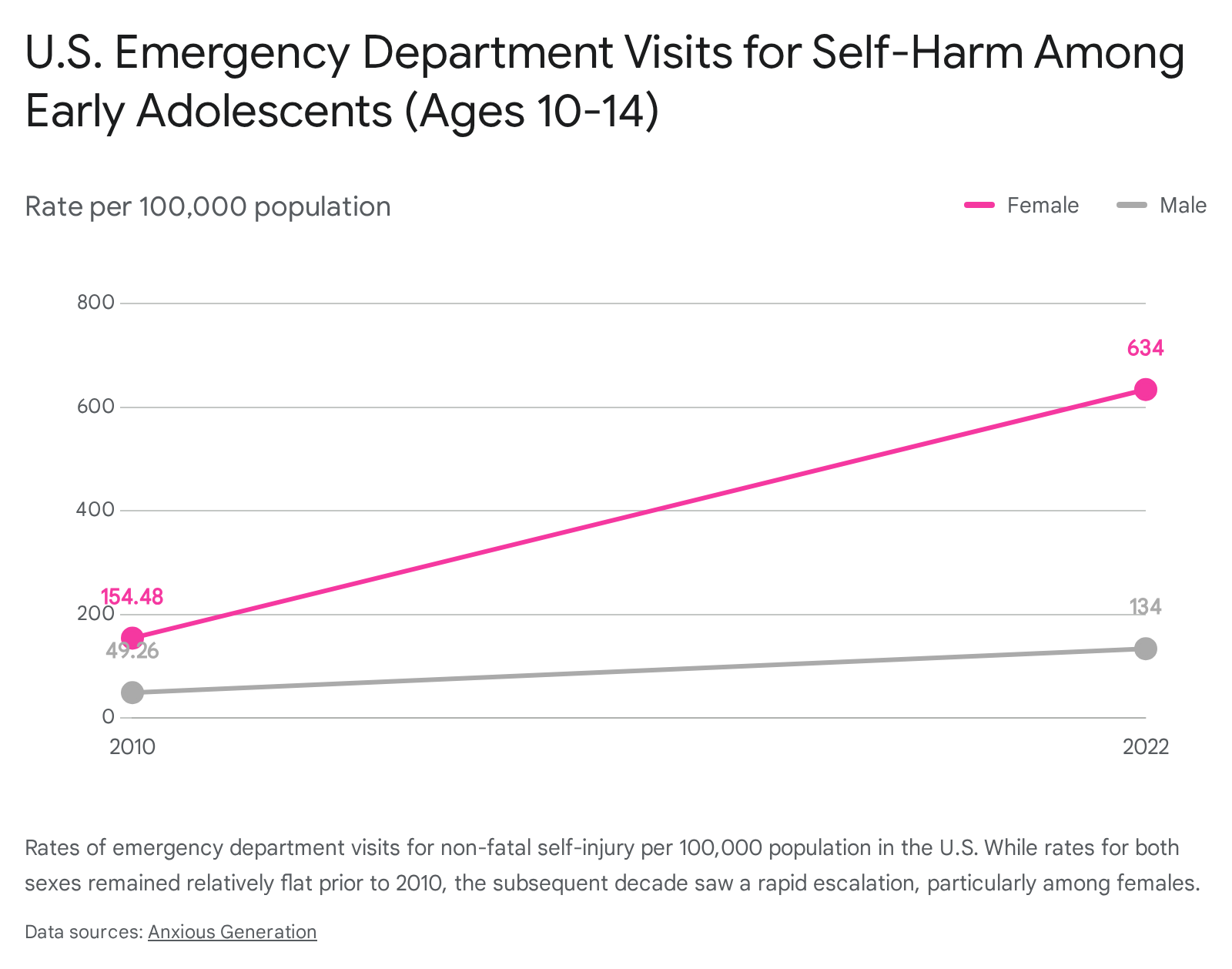
The compounding nature of this distress is evident in healthcare utilization barriers; among adolescents with a current diagnosis who required treatment, 61.0% experienced difficulty accessing care in 2023, representing a 35% increase in access barriers since 2018 2.
Trajectories in East Asian Populations
The upward trend is similarly observable in East Asia. In China, a national psychiatric epidemiological survey of 17,524 school-aged children and adolescents reported an overall mental health disorder prevalence of 17.5% 3. A 2022 large-scale provincial screening in Jiangsu Province involving 123,005 students found that 14.6% of the population exhibited depression symptoms, 8.0% exhibited clinical anxiety, and 27.4% demonstrated signs of severe stress 34. The prevalence of these conditions scaled with age, indicating that upper secondary students preparing for university entrance examinations bear the highest burden of internalizing disorders 4.
South Korea demonstrates arguably the steepest recent trajectory in the region. Clinical treatment registries recorded a 65.2% increase in teenagers receiving treatment for anxiety disorders between 2020 and 2024, rising from 25,192 to 41,611 patients 5. Most concerning from a developmental perspective is that the incidence surge was steepest among children under the age of 10, which saw an 87.6% increase in anxiety treatments over the same four-year window 5. The incidence of clinical depression in South Korean children under 10 concurrently jumped 118.2% from 2020 to 2024, highlighting a profound deterioration in early childhood psychological stability 6.
Emerging Vulnerabilities in Low- and Middle-Income Regions
While the GBD 2021 study notes that regions with a High Socio-Demographic Index (SDI) experienced the largest proportional increases in incidence over the past 30 years, Middle SDI regions currently report the highest absolute number of cases 1. Emerging economies face profound vulnerabilities regarding adolescent mental health, often exacerbated by scarce clinical infrastructure.
In sub-Saharan Africa, an estimated 14% of adolescents experience a mental health disorder 7. A study utilizing data from the African Research, Implementation Science, and Education (ARISE) Network analyzed nearly 10,000 adolescents and found the highest risk profiles among older adolescents from low-income households with histories of physical injury 7. Focused regional studies underscore this severity: a recent assessment of young adolescents (aged 10 - 14) in the Western Cape of South Africa found that 33% reported symptoms of depression and 21% reported symptoms of anxiety 8. Structural equation modeling applied to South African cohorts reveals that demographic determinants such as extreme poverty, food insecurity, and caregiver absence act as direct drivers of clinical anxiety in these populations 88.
Divergent Trends in Eastern Europe and Central Asia
The global dataset is not entirely monolithic. Some regions exhibit stability in youth mental health relative to historical baselines. Analyses combining the Gallup World Poll, Eurobarometers, and the European Social Survey indicate that the mental health of youth relative to older populations has remained stable across much of Eastern Europe and Central Asia, including many post-Soviet republics 9. In these regions, the traditional "U-shape" of psychological well-being (where well-being dips in middle age and is higher in youth and old age) remains largely intact, standing as a notable outlier to the dominant Western and East Asian trends where youth well-being has plummeted below that of older adults 9.
| Geographic Region | Metric / Data Point | Timeframe | Sub-Population Variances |
|---|---|---|---|
| Global (GBD) | 52.0% increase in incident cases of anxiety | 1990 - 2021 | Highest proportional increases in High SDI regions; 20-24y age group saw largest total rise 1. |
| United States | 61.0% increase in diagnosed anxiety | 2016 - 2023 | 20.1% female prevalence vs. 12.3% male prevalence 2. |
| South Korea | 65.2% increase in anxiety disorder treatments | 2020 - 2024 | 87.6% clinical increase observed in children under age 10 5. |
| China | 14.2% - 17.5% baseline prevalence of anxiety | 2022 - 2023 | Symptoms highest among senior secondary students facing academic transitions 310. |
| South Africa | 21.0% prevalence of anxiety symptoms (Western Cape) | 2023 - 2024 | Rates mediated strongly by food insecurity and exposure to adult violence 88. |
The Technological Displacement Framework
A prominent explanatory framework for the post-2010 rise in adolescent internalizing disorders focuses on the ubiquitous adoption of smartphones and algorithmic digital media. Spearheaded by researchers examining population time-diary studies, this hypothesis posits that the rapid transition from physical socialization to screen-mediated interaction fundamentally disrupted the behavioral and neurological development of a demographic cohort 1112.
Digital Media Engagement and Sleep Disruption
Longitudinal time-use data indicates a steep decline in the minutes per day adolescents spend socializing in person, which inversely tracks with the rise of digital media consumption 1314. This displacement of physical interaction strips adolescents of synchronous behavioral cues, tactile contact, and real-time conflict resolution practices, all of which serve as natural regulatory mechanisms against anxiety and isolation 1114.
Furthermore, digital media use acts as a profound disruptor of adolescent sleep architecture. Meta-analyses of problematic social media use demonstrate a consistent, deleterious effect on sleep quality, latency, and duration 151617. The relationship operates through a recognized "serial mediation model": high emotional investment in social media platforms leads to negative social comparisons, which subsequently triggers pre-sleep cognitive arousal and rumination, ultimately resulting in insomnia symptoms 1819. Because adequate sleep is critical for emotional regulation and cognitive resilience, its systemic truncation - where adolescents trade restorative rest for screen time - leaves them biologically vulnerable to anxiety and depressive spirals 111319. Canadian public health data corroborates this mechanism, demonstrating that non-active social media use is associated with better sleep health, while problematic use correlates with adjusted odds ratios up to 3.24 for poor sleep indicators 17.
Neurobiological Mechanisms and Algorithmic Vulnerability
Beyond behavioral displacement, the architecture of social media platforms directly interfaces with adolescent neurobiology. Platforms optimize for continuous engagement using variable reward schedules - the same psychological mechanisms utilized to foster behavioral addiction in gambling environments 20. The adolescent brain responds not merely to the receipt of a social reward (e.g., a "like" or comment), but to the anticipation and algorithmic uncertainty of that reward, which triggers potent dopamine release along the brain's reward pathways 2021.
During adolescence, the brain is highly plastic and characterized by an asymmetrical developmental timeline: the reward system (the striatum) matures rapidly, while the cognitive control system (the prefrontal cortex) develops much more slowly 2123. Frequent engagement with highly optimized, AI-driven feeds artificially elevates baseline dopamine levels. Over time, this chronic overactivation leads to dopamine receptor downregulation, manifesting as reduced reward sensitivity 2123. Consequently, natural, lower-dopamine activities (such as reading, physical play, or offline socialization) become anhedonic, driving the adolescent back to the high-stimulus digital environment to maintain homeostasis 22.
Neurological imaging of heavy adolescent social media users indicates structural and functional alterations, including decreased gray matter density and reduced responsiveness in the dorsolateral prefrontal cortex (dlPFC) - the region responsible for executive function, impulse control, and emotional regulation 2021. This compromised top-down regulation leaves adolescents hypersensitive to social rejection and peer comparison, effectively lowering the neurological threshold for anxiety disorders.
Methodological Contestation Regarding Technology Claims
While the technological displacement framework has gained broad cultural traction, the empirical evidence linking digital media to clinical anxiety remains highly contested within the scientific community. The debate hinges largely on the interpretation of large correlational datasets.
Researchers investigating the exact same datasets have arrived at starkly different conclusions based on their statistical methodologies. Critics of the technological framework argue that analyses often fail to distinguish between active, passive, and problematic digital use, treating "screen time" as a monolith 23. Some large-scale analyses have concluded that the negative association between digital technology use and adolescent mental health is minuscule - statistically comparable in effect size to wearing glasses or regularly eating potatoes 23.
Conversely, proponents of the technological framework argue that these specific analyses dilute the data by grouping benign screen time (e.g., watching educational videos, video chatting with family) together with highly algorithmic social media use 23. When isolating specifically for social media engagement among female adolescents, researchers identify a much stronger negative association with mental health outcomes, comparable to the effect sizes associated with binge drinking or hard drug use 23. The lack of definitive longitudinal randomized controlled trials leaves the exact causal direction - whether social media causes anxiety, or whether anxious adolescents retreat to social media - a subject of calibrated uncertainty in the current literature.
Escalation of Academic Demands and Educational Stress
Concurrent with technological shifts, the intensification of global academic standards and the commercialization of educational success have emerged as major structural stressors for adolescents. The modern educational environment increasingly ties an adolescent's future socioeconomic survival to high-stakes testing, fostering chronic psychological strain.
Transnational Increases in Schoolwork Pressure
A comprehensive 2024 report by the World Health Organization (WHO) and the Health Behaviour in School-aged Children (HBSC) study tracked the well-being of nearly 280,000 adolescents across 44 countries in Europe, Central Asia, and Canada 2425. The longitudinal data paints a stark picture of rising academic anxiety paired with eroding social safety nets. In 2022, 63% of 15-year-old girls reported feeling pressured by schoolwork - a substantial jump from 54% in the previous 2018 survey 24. Boys reported a similar, though less acute, increase in academic pressure (rising from 40% to 43%) 24.
Hierarchical multilevel models evaluating cross-national time trends between 2002 and 2018 confirmed that even prior to the pandemic, increases in schoolwork pressure partially explained the corresponding rise in psychosomatic health complaints among adolescents in high-income countries 2627.
The Hyper-Competitive East Asian Model
The psychological toll of academic burden is particularly quantifiable in East Asian educational systems, which are characterized by intense structural competition. In South Korea, academic pressure is recognized as the primary driver of the country's severe youth mental health crisis and its uniquely high adolescent suicide rate 28. The structural integration of private "cram schools" (Hagwons) extends the typical academic day to between 12 and 16 hours 28. Hyper-visible peer ranking systems, where report cards display student ranks within the school, induce chronic fears of inferiority 28. A 2024 survey of 10,140 South Korean students calculated a "children's happiness index" of merely 45.3 out of 100, which dropped to 44.16 among those experiencing acute study pressure 5.
Similarly, in China, structural equation modeling applied to longitudinal cohort studies reveals how academic burden maps directly onto psychopathology. A study of Chinese adolescents (n=2,965) tracked the pathways from academic stress to clinical anxiety and depression across three time points in 2022 and 2023 29. The analysis found that the relationship is significantly mediated by sleep deprivation and loneliness. Academic stress degrades sleep duration and quality, a mediation effect that accounted for 34.4% of the total indirect pathway driving anxiety symptoms 29. The resulting social isolation (loneliness) accounted for another 20.8% of the pathway to anxiety 29. These findings illustrate how structural educational demands force behavioral compromises that organically produce clinical anxiety.
Disintegration of Social Support Structures
The rise in academic stress has been compounded by a concurrent weakening of the social frameworks necessary to buffer that stress. The WHO/HBSC report indicates that between 2018 and 2022, the proportion of adolescents reporting high levels of family support dropped from 73% to 68% 2425. Peer support simultaneously fell from 61% to 58% 24. This decline was most pronounced among female adolescents, whose perception of strong family support fell from 72% to 64% over just four years 2425. The erosion of these core protective factors leaves adolescents highly exposed to the psychological friction of modern academic environments.
| Intermediary Variable | Mediation Effect on Depression | Mediation Effect on Anxiety | Mechanism Description |
|---|---|---|---|
| Sleep Quality/Duration | 30.8% of total indirect effect | 34.4% of total indirect effect | Academic demands strictly reduce hours available for sleep, impacting cognitive recovery 29. |
| Loneliness | 26.7% of total indirect effect | 20.8% of total indirect effect | High study volume limits physical peer interaction, reducing social regulatory buffers 29. |
| Physical Activity | 1.9% of total indirect effect | Not statistically significant | Sedentary study habits displace exercise, minimally impacting anxiety but affecting mood 29. |
Note: Mediation data derived from 2022 - 2023 structural equation modeling of Chinese adolescent cohorts.
Macroeconomic Instability and Megatrends
The psychiatric epidemiology of youth cannot be decoupled from broader macro-historical contexts. The 2024 Lancet Psychiatry Commission on Youth Mental Health identifies a convergence of structural "megatrends" that are fundamentally undermining the psychological security of emerging adults on a global scale 303132.
Intergenerational Precarity and the Polycrisis
The Commission posits that adolescents serve as sensitive barometers of societal instability. Interconnected commercial and socioeconomic forces - including the existential threat of climate change, widening intergenerational wealth inequality, declining social cohesion, and acute housing and financial precarity - generate a pervasive sense of a "bleak future" 3334.
This macro-anxiety acts as a chronic background stressor, maintaining the adolescent nervous system in a state of continuous, low-level hyperarousal. Unlike acute, localized threats that can be fought or fled, systemic issues like economic precarity offer adolescents little to no locus of control. The result is a high prevalence of generalized anxiety and hopelessness. The Lancet Commission emphasizes that traditional clinical models (e.g., individual psychiatric therapy) are fundamentally insufficient to treat epidemiological spikes caused by systemic socioeconomic failures; a preventative public health approach addressing the root social determinants of health is required 303134.
The COVID-19 Pandemic as a Catalytic Event
The COVID-19 pandemic acted as an unprecedented catalyst, sharply exacerbating the pre-existing baseline of rising anxiety and depression. Global school closures severed adolescents from vital peer networks, extracurricular structures, and school-based mental health services, while simultaneously driving unprecedented spikes in sedentary screen time and sleep disruption 3536.
In the U.S., electronic health record data spanning 2017 to 2023 demonstrated the acute impact of this disruption. Average monthly primary care visits resulting in anxiety diagnoses increased by 71% for adolescent females (aged 12-17) and 62% for males when comparing pre-pandemic to post-pandemic periods 37. Medical emergency departments experienced a 50% increase in youth presentations for suicidal ideation and self-harm between 2019 and 2022, leading to a critical capacity crisis due to the lack of available inpatient psychiatric beds 38.
Post-Pandemic Trajectories and Clinical Reversions
However, careful longitudinal analysis indicates that the pandemic amplified, rather than initiated, the youth mental health crisis. Out of nine major longitudinal studies evaluating the pandemic's impact on youth, seven reported rising anxiety and depression rates well before the pandemic began 39.
Most critically, post-pandemic data offers nuanced insights into the reversibility of acute distress. Electronic health records indicate that after peaking during the immediate wake of the pandemic, monthly rates of anxiety and mood disorder diagnoses began to significantly decrease throughout 2022 and 2023 37. Studies specifically tracking school reopenings found that by the ninth month of returning to in-person education, overall mental health diagnoses among children dropped by 1.2 percentage points, with significant reductions in depression and medical costs - particularly for female students 36. This empirical reversion reinforces the hypothesis that structural routines, physical socialization, and separation from constant digital engagement act as primary psychiatric stabilizers for youth.
The Prevalence Inflation Hypothesis
While the epidemiological data unequivocally shows more adolescents reporting anxiety and entering clinical treatment, an emerging paradigm questions whether the underlying rates of true clinical pathology have risen as steeply as the self-reported data suggests. Spearheaded by researchers evaluating the cultural framing of distress, the "prevalence inflation hypothesis" offers a critical counterweight to purely structural or technological explanations.
Expansion of Diagnostic Thresholds and Overinterpretation
Over the last decade, intense public health and cultural efforts have focused on destigmatizing mental illness and increasing mental health literacy. The prevalence inflation hypothesis suggests these well-intentioned awareness efforts have yielded a paradoxical dual outcome 404142.
The beneficial outcome is improved recognition: individuals who previously suffered in silence with legitimate psychiatric disorders are now equipped with the vocabulary to seek diagnosis and treatment 4142. The problematic outcome, however, is overinterpretation. Widespread awareness campaigns and the proliferation of therapeutic language in digital spaces have led adolescents to interpret milder, normative forms of human distress - such as exam anxiety, social awkwardness, or temporary sadness - as symptoms of medicalized psychiatric disorders 404143.
The Contagion of Terminology and Self-Fulfilling Dynamics
This semantic shift becomes clinically relevant through the mechanism of a self-fulfilling prophecy. When an adolescent labels standard psychological discomfort as a clinical "anxiety disorder," it fundamentally alters their self-concept and drives maladaptive behavioral modifications 40414344. For instance, a teenager who views mild nervousness as indicative of an anxiety disorder may begin systematically avoiding challenging social or academic situations. This behavioral avoidance prevents the individual from building resilience and habituating to normative stressors, thereby allowing genuine, pathological anxiety to take root where only transient distress previously existed 414445.
Evidence of Iatrogenic Harm in Universal Interventions
The prevalence inflation framework extends to direct critiques of modern educational policy, specifically the implementation of universal school-based mental health interventions. These programs, which often teach cognitive behavioral therapy (CBT) skills or mindfulness to entire classrooms regardless of baseline symptomology, may be causing iatrogenic harm - adverse effects resulting directly from the treatment itself 46494748.
In several randomized controlled trials and meta-analyses, students subjected to universal mental health interventions reported an increase in internalizing symptoms relative to control groups who simply attended regular academic lessons 4947. Researchers identify two primary mechanisms for this harm: 1. Rumination: By forcing non-symptomatic adolescents to hyper-focus on identifying, tracking, and analyzing negative emotions, interventions inadvertently encourage a pathological dwelling on distress 47. 2. Deviancy Training (Peer Influence): Delivering interventions in group settings allows adolescents to co-ruminate. Vulnerable students may adopt the negative thought patterns, psychiatric labels, or maladaptive coping mechanisms vocalized by their peers, inadvertently spreading distress contagiously through the cohort 4947.
The prevalence inflation framework does not dismiss the suffering of modern youth; rather, it suggests that the current cultural and clinical apparatus designed to monitor adolescent mental health may be accidentally manufacturing a portion of the clinical anxiety it seeks to eradicate.