Clinical evidence for fasting-mimicking diets
The pursuit of longevity and the mitigation of age-related cardiometabolic and neoplastic diseases have driven extensive research into dietary restriction protocols. Chronic caloric restriction and profound water-only fasting are well-documented interventions capable of extending lifespan and healthspan in various model organisms by targeting fundamental cellular aging mechanisms. However, the rigorous demands of chronic caloric restriction and the potential physiological hazards of prolonged water fasting - such as severe lean muscle mass depletion, malnutrition, and impaired immune function - render these protocols largely infeasible and potentially unsafe for the general human population.
In response to these substantial clinical limitations, the fasting mimicking diet (FMD) was developed to trigger the physiological and cellular benefits of prolonged fasting without requiring absolute caloric deprivation. Conceptualized and refined by Valter Longo and researchers at the University of Southern California Longevity Institute, with foundational funding from the National Institute on Aging (NIA) and the National Cancer Institute (NCI), the fasting mimicking diet is a periodic, plant-based nutritional intervention 12. It is meticulously designed to suppress nutrient-sensing pathways and induce a fasting state at the cellular level while safely supplying essential macronutrients and micronutrients. Emerging clinical and preclinical data indicate that brief, repeated cycles of the fasting mimicking diet can modulate systemic inflammation, reverse cardiometabolic risk factors, enhance the efficacy of antineoplastic therapies, and significantly reduce biomarkers associated with biological aging.
Foundational Principles and Nutrient-Sensing Pathways
The therapeutic efficacy of the fasting mimicking diet relies on the precise manipulation of dietary macronutrients to alter systemic energy metabolism and intracellular signaling cascades. By circumventing complete starvation, the diet sustains basal physiological functions while initiating systemic repair protocols that are evolutionarily conserved from yeast to mammals.
Suppression of Pro-Aging Cellular Pathways
The primary biochemical objective of the fasting mimicking diet is the profound downregulation of major nutrient-sensing pathways, particularly the insulin-like growth factor 1 (IGF-1) pathway, the mechanistic target of rapamycin (mTOR), and protein kinase A (PKA) 345. Preclinical genetic studies and epidemiological observations confirm that high circulating levels of IGF-1 and the hyperactivation of the mTOR/Tor-S6K pathways are strongly correlated with accelerated cellular aging, neoplastic proliferation, and insulin resistance 23.
Dietary amino acids - particularly essential amino acids - are potent stimulators of the mTOR pathway, while simple carbohydrates and high caloric loads drive glucose and insulin spikes that activate IGF-1 and PKA. By severely restricting protein and overall caloric intake, the fasting mimicking diet significantly reduces circulating IGF-1 while simultaneously increasing the production of insulin-like growth factor-binding protein 1 (IGFBP-1), a protein that binds to and further inhibits IGF-1 signaling 46. This orchestrated suppression shifts somatic cells away from active growth and division, redirecting cellular energy toward stress resistance and repair.
Macronutrient Formulation and Metabolic Shift
The fasting mimicking diet is typically administered in five-day cycles, utilized once per month for three to six consecutive months, depending on the specific clinical objective or baseline patient health. The dietary composition is strictly standardized to maintain low caloric density, low protein, and low carbohydrate intake, alongside a relatively high proportion of plant-based unsaturated fats.
During the five-day intervention, normal food is entirely replaced by a proprietary or standardized vegan protocol consisting of soups, energy bars, and herbal teas. The regimen is designed to rapidly deplete hepatic glycogen stores, lower circulating glucose, and force the body into a state of ketosis, thereby elevating the production of ketone bodies such as beta-hydroxybutyrate, which serve as an alternative fuel for the brain and peripheral tissues 178.
| Fasting Mimicking Diet Phase | Caloric Intake | Carbohydrates | Fats | Protein | Primary Physiological Objective |
|---|---|---|---|---|---|
| Day 1 (Transition) | ~1,100 kcal | 34% | 56% | 10% | Initiate hepatic glycogen depletion and transition toward lipid oxidation 3. |
| Days 2 - 5 (Mimicry) | ~725 - 800 kcal | 47% | 44% | 9% | Sustain ketosis, suppress IGF-1/mTOR pathways, and induce autophagic flux 3. |
| Days 6 - 30 (Refeeding) | Ad libitum / Healthy | Variable | Variable | Variable | Stimulate stem cell proliferation and tissue regeneration upon nutrient reintroduction 59. |
The protein sources utilized in the diet are exclusively plant-based to minimize the intake of specific essential amino acids that independently trigger growth pathways 1. This specific macronutrient ratio ensures that despite the ingestion of physical matter, the body's nutrient-sensing mechanisms remain largely inactive, thus mimicking the systemic signature of a water-only fast.
Cellular Autophagy and Immune Dynamics
A hallmark consequence of nutrient pathway suppression is the induction of autophagy - a highly conserved cellular recycling process wherein damaged organelles, misfolded proteins, and intracellular debris are encapsulated and degraded. While autophagy has been exhaustively studied in animal models, translating these molecular dynamics into human clinical trials has historically proven difficult.
Autophagic Flux and LC3B Dynamics
Recent advancements have allowed researchers to directly quantify autophagic flux in human subjects undergoing periodic dietary restriction. A pivotal 2026 randomized controlled trial conducted by researchers at Cedars-Sinai Medical Center and UT Health San Antonio investigated the cellular effects of the fasting mimicking diet in 30 healthy adults 81011. The study assigned participants to either a standard FMD formulation (ProLon), a modified formulation (FMD2), or an unrestricted control diet.
By analyzing the dynamics of the microtubule-associated protein 1A/1B-light chain 3B (LC3B) within immune cells across multiple time points, researchers were able to measure the rate of autophagosome degradation. The data indicated an acceleration of autophagic turnover rather than mere static accumulation of autophagic proteins 8. The trial demonstrated that the standard five-day fasting mimicking diet induced a measurable increase in autophagic flux that remained detectable up to two days into the refeeding period (day eight of the trial cycle) 8. This suggests that brief, severe dietary stress can durably recalibrate cellular maintenance systems, extending biological benefits beyond the strict fasting window.
Immunological Rejuvenation and Stem Cell Activation
The intermittent nature of the diet - a period of restriction followed by a robust refeeding phase - is vital to its regenerative capacity. During the fasting phase, the body breaks down damaged cellular debris, misfolded proteins, and non-essential tissues to synthesize energy. This process often includes the targeted apoptosis of senescent cells and damaged immune cells 511.
Upon refeeding, the sudden influx of nutrients activates dormant stem cells to rebuild the depleted tissues. This cyclic fasting-and-refeeding mechanism has been shown to facilitate multi-system regeneration. Clinical assessments of individuals completing multiple cycles of the fasting mimicking diet consistently reveal an improved lymphoid-to-myeloid cell ratio, indicating a profound rejuvenation of the immune system profile, which typically skews toward myeloid dominance as individuals age 1112.
Cardiometabolic and Endocrine Applications
The metabolic shift precipitated by the fasting mimicking diet translates into profound systemic changes, particularly in the management of cardiometabolic risk factors. The diet's ability to reduce central adiposity, modulate insulin dynamics, and improve lipid profiles positions it as a potent non-pharmacological intervention for metabolic syndrome and type 2 diabetes.
Glycemic Control and Type 2 Diabetes Management
Clinical trials examining the fasting mimicking diet in patients with prediabetes and type 2 diabetes have demonstrated acute and sustained improvements in glycemic regulation. A single five-day cycle rapidly decreases fasting glucose by approximately 13 to 14 mg/dL and concurrently decreases circulating insulin levels, establishing an immediate enhancement of insulin sensitivity 8.
In longer-term interventions, the physiological reset provided by periodic fasting yields highly durable benefits. A 2025 real-world study evaluating an up-to-eight-month FMD program in patients with type 2 diabetes found that the proportion of participants achieving a hemoglobin A1c (HbA1c) level below 7% increased significantly from 49% at baseline to 70% at three months, stabilizing at 62% by the six-month mark 14. Furthermore, 73% of participants were able to reduce their diabetes medication dosages at three months, demonstrating the clinical viability of the diet in reducing pharmacologic dependency 314.
These outcomes contrast favorably with traditional dietary interventions. Direct comparative analyses against continuous Mediterranean diets have revealed that while continuous adherence to a Mediterranean diet promotes gradual metabolic health, brief five-day cycles of the fasting mimicking diet are markedly superior at rapidly reversing insulin resistance. In cross-over trials, a five-day continuous Mediterranean diet failed to alter insulin resistance, whereas the fasting mimicking diet reduced Homeostatic Model Assessment for Insulin Resistance (HOMA-IR) scores dramatically from 6.4 to 2.6 13.
Adiposity, Hepatic Fat, and Body Composition
Weight reduction resulting from the fasting mimicking diet is driven predominantly by the targeted depletion of visceral and hepatic fat, with multiple studies documenting marked reductions in waist circumference and overall body mass index (BMI) 31215. Participants in metabolic tracking trials routinely record an average weight loss of 1.7 kilograms following a single five-day cycle, while mid-term three-to-six-month protocols yield aggregate weight reductions averaging 4.5 to 6.7 kilograms 814. Magnetic resonance imaging has further confirmed that the diet aggressively depletes hepatic fat fractions, establishing it as a highly promising therapeutic intervention for non-alcoholic fatty liver disease (NAFLD) and related hepatic steatosis 111213.
Comparative Efficacy of Dietary Restriction Protocols
It is highly illustrative to contrast the fasting mimicking diet with other contemporary dietary restriction paradigms, such as continuous energy restriction (CER), alternate-day fasting (ADF), and time-restricted eating (TRE). While all methodologies induce weight loss via caloric deficits, their specific metabolic mechanisms, clinical implementation, and long-term adherence profiles differ substantially.
| Dietary Protocol | Typical Implementation | Primary Metabolic Mechanism | Expected Weight Loss | Long-Term Adherence Challenges |
|---|---|---|---|---|
| Fasting Mimicking Diet (FMD) | 5 days of severe restriction (725-1100 kcal) per month; 25 days ad libitum. | Downregulation of IGF-1/mTOR, profound ketosis, stem cell activation. | 1.7 kg per cycle; 4.5 - 6.7 kg over 6 months 814. | High feasibility due to episodic nature; avoids chronic daily fatigue 914. |
| Alternate-Day Fasting (ADF) | 24 hours of extreme restriction (0-25% needs) alternating with 24 hours ad libitum. | Intermittent glycogen depletion and sustained overall caloric deficit. | 3% - 12.9% over 3 to 12 weeks 1418. | Poor long-term sustainability; frequent hunger on fast days disrupts social eating and habits 1520. |
| Time-Restricted Eating (TRE) | Daily eating compressed to 4 - 10 hours (e.g., 16:8); daily prolonged fasting. | Circadian rhythm alignment, increased nocturnal lipid oxidation. | 0.9% - 8.6% depending on spontaneous caloric reduction 1816. | Highly sustainable, but the 2026 ChronoFast study shows no metabolic benefit if overall calories are not reduced 171819. |
| Continuous Energy Restriction (CER) | Daily caloric deficit of 400 - 750 kcal across all meals. | Sustained negative energy balance. | 5% - 10% of body weight over 6 months 2021. | High attrition rates due to diet fatigue, adaptive thermogenesis, and chronic hunger 222324. |
Blood Pressure and Cardiovascular Lipids
The cardiovascular benefits of the fasting mimicking diet extend beyond glucose and adipose metabolism. Intervention cohorts consistently demonstrate significant reductions in both systolic and diastolic blood pressure, particularly among individuals presenting with baseline hypertension 36. A 2025 meta-analysis of randomized controlled trials confirmed that the fasting mimicking diet reduces systolic blood pressure by a weighted mean difference of 4.15 mmHg and diastolic blood pressure by 2.26 mmHg 6. The lipid profile often shows highly favorable modifications, including reductions in circulating triglycerides and total cholesterol, contributing to an overall decline in systemic cardiovascular risk 122526.
Gastrointestinal Pathology and Microbiome Shifts
The gastrointestinal tract represents a major interface for the immunomodulatory effects of the fasting mimicking diet. Chronic, low-grade inflammation is a primary driver of numerous systemic conditions, but when localized to the gut, it manifests as inflammatory bowel diseases (IBD), including Crohn's disease and ulcerative colitis, characterized by hyperactive mucosal immune responses and microbial dysbiosis.
Efficacy in Crohn's Disease
A landmark 2026 randomized controlled trial involving 97 patients with mild to moderate Crohn's disease assessed the efficacy of integrating three cycles of the fasting mimicking diet alongside standard pharmacological care. The dietary intervention demonstrated profound clinical utility in achieving disease remission.
The trial reported that 69% of the patients receiving the diet achieved a clinically significant improvement in Crohn's symptoms and attained clinical remission, compared to only 44% in the control group receiving standard pharmaceutical care alone 127.
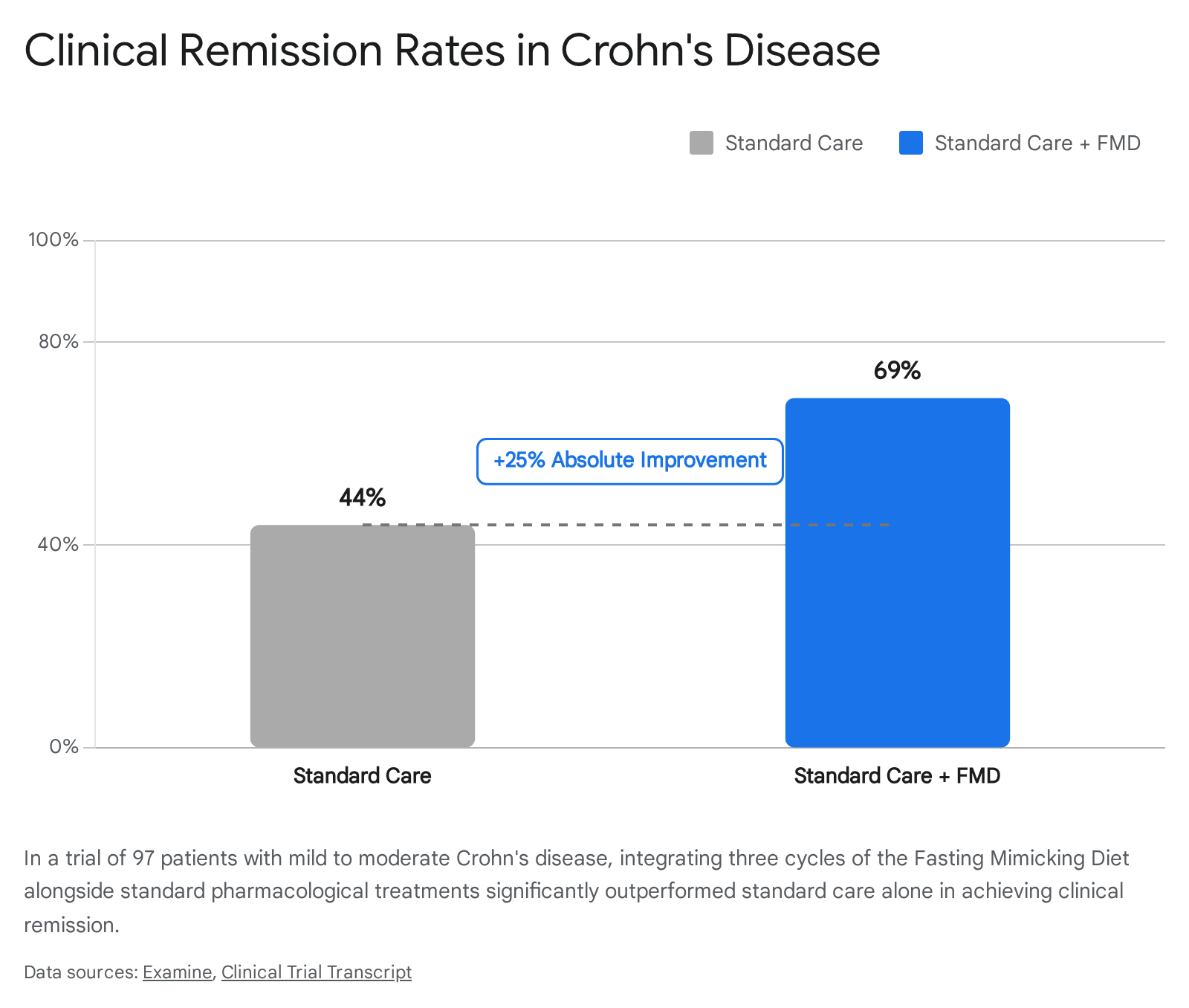
Furthermore, the dietary cohort exhibited significant reductions in fecal calprotectin, a direct and reliable biomarker of intestinal mucosal inflammation 127. While the FMD group experienced minor, transient adverse effects such as headache, fatigue, and bloating during the five-day cycles, the intervention was broadly well-tolerated 27.
Prebiotic Optimization over Water Fasting
The superiority of the fasting mimicking diet over traditional water-only fasting in the context of gastrointestinal health relates heavily to its precise macronutrient and fiber design. Preclinical models of IBD have demonstrated that water-only fasting, while broadly anti-inflammatory, fails to optimally support mucosal regeneration due to the complete absence of prebiotic substrates. The fasting mimicking diet circumvents this by including specific plant-based prebiotics that actively reshape the gut microbiota.
Following the intervention, researchers observed a pronounced expansion of beneficial bacterial populations, notably Lactobacillaceae and Bifidobacteriaceae 128. This microbial shift promotes the generation of short-chain fatty acids, enhances intestinal stem cell activation, and facilitates a more robust regeneration of the intestinal epithelium than traditional fasting protocols 128.
Oncological Applications and Tumor Metabolism
The integration of targeted dietary strategies into oncology represents a paradigm shift in cancer therapeutics. Fasting mimicking diets are being actively evaluated for their potential to drastically alter the tumor microenvironment, exploiting the metabolic inflexibility inherent to most malignant cells.
Differential Stress Resistance
The application of FMD in oncology relies heavily on a biological mechanism known as differential stress resistance. Under the physiological stress of the fasting mimicking diet, healthy somatic cells enter a shielded, highly conserved maintenance state via the downregulation of IGF-1 and mTOR pathways 24. In this state, normal cells halt active division and redirect energy toward DNA repair and oxidative defense.
Conversely, malignant cells, driven by potent oncogenic mutations, are incapable of halting their proliferation pathways despite the lack of circulating nutrients. Consequently, they fail to enter a protective maintenance state. This biological divergence leaves malignant cells unshielded and actively attempting to grow in a resource-depleted environment. As a result, cancer cells exhaust their metabolic resources and become highly susceptible to oxidative stress, DNA damage, and apoptosis, while the surrounding healthy tissues remain heavily protected against toxic insults 24.
Chemosensitization and Immunotherapy Synergies
Preclinical research has thoroughly evaluated the fasting mimicking diet across a myriad of experimental cancer models. A comprehensive 2026 systematic review published in the European Journal of Nutrition confirmed that the diet, when utilized as a standalone intervention, significantly delays tumor progression, downregulates tumor-promoting biomarkers, and restricts metastatic proliferation 429.
However, the diet's most profound application is as a therapeutic adjuvant. When cycles of the fasting mimicking diet are administered concomitantly with cytotoxic chemotherapy, targeted kinase inhibitors, or hormone therapy, the resultant nutrient scarcity exacerbates the oxidative stress inside malignant cells, preventing them from repairing the DNA damage inflicted by the drugs 24. Recent advancements point toward potent synergies with immunotherapy; by alleviating local immunosuppression and stimulating anti-tumor immunity, the diet improves the efficacy of advanced therapies such as anti-PD1 checkpoint inhibitors 235.
| Oncological Therapy Class | Mechanism of Synergy with Fasting Mimicking Diet | Preclinical/Clinical Outcomes |
|---|---|---|
| Cytotoxic Chemotherapy | DSR protects healthy cells from toxicity while starving cancer cells of glucose needed for rapid division 4. | Reduced hematological toxicity, preserved healthy tissue, enhanced tumor apoptosis 24. |
| Immunotherapy (Anti-PD1) | Reduces systemic inflammation and remodels the tumor microenvironment to favor immune cell infiltration 435. | Heightened anti-tumor immunity, overcoming resistance to checkpoint inhibitors 235. |
| Targeted Therapy / Kinase Inhibitors | Prevents cancer cells from utilizing alternative metabolic escape pathways when primary kinases are blocked 4. | Delayed onset of drug resistance, prolonged progression-free survival in models 4. |
Preclinical to Clinical Translation
While the preclinical data is exceptionally robust, translating these findings into standardized oncological practice requires overcoming distinct clinical hurdles. Systematic reviews underscore significant heterogeneity across human oncology trials regarding protocol duration, the number of dietary cycles administered, and variations in therapeutic drug combinations 4. Furthermore, managing dietary compliance among oncology patients who may already be experiencing cancer-related cachexia or treatment-induced anorexia requires meticulous clinical and nutritional oversight 30. Consequently, while the fasting mimicking diet shows substantial promise for reprogramming tumor metabolism and improving quality of life during chemotherapy, it is currently utilized primarily within the boundaries of controlled clinical trials rather than as an independent standard of care.
Longevity and Biological Age Biomarkers
At its core, the formulation of the fasting mimicking diet is rooted in the science of gerontology. By intermittently clearing senescent cells, dampening systemic inflammation, and preserving metabolic elasticity, the diet addresses the fundamental biological drivers of the aging process, offering interventions that target lifespan extension at the cellular level.
Reversal of Biological Clocks
Chronological age is an immutable metric, but biological age - a measure of cellular and tissue functionality - is dynamic and responsive to environmental, behavioral, and nutritional inputs. Leveraging comprehensive clinical biomarker datasets, such as the Third National Health and Nutrition Examination Survey (NHANES) and the CALERIE trials, researchers have established validated composite biological age scores that are highly predictive of morbidity and mortality 1213.
In clinical trials involving diverse adults aged 18 to 70, participants completing just three monthly cycles of the fasting mimicking diet exhibited a median biological age reduction of 2.5 years 91112. This calculation factors in a multitude of systemic improvements: the reversal of immune system aging, the profound reduction of hepatic fat, the stabilization of glycemic control, and reductions in systemic inflammatory markers like CRP 1213. Crucially, complex statistical analyses demonstrate that this age-reversing effect operates independently of overall body weight loss, proving that the benefits stem from deep cellular reprogramming and autophagic clearance rather than the mere mechanics of a caloric deficit 1113. Predictive modeling suggests that integrating periodic fasting cycles into routine care from age 50 could significantly extend life expectancy, potentially adding up to five years of healthy longevity 13.
To validate these findings on a larger scale, extensive longitudinal trials are currently underway. Notably, a randomized trial (NCT07255300) initiated in 2024 is tracking 501 adult subjects over six months to assess the long-term trends of the fasting mimicking diet, both alone and in combination with a continuous "Longevity Diet," measuring hard endpoints of body composition and biological aging biomarkers 31.
Contraindications and Clinical Limitations
Despite its diverse metabolic, immunomodulatory, and gerontological benefits, the fasting mimicking diet is not universally appropriate. The intervention imposes acute physiological stress that can be detrimental to specific clinical populations if misapplied without proper medical screening.
Sarcopenia and Lean Muscle Mass Attrition
A prevailing and severe critique of profound weight-loss interventions - including daily caloric restriction, bariatric surgery, and modern GLP-1 receptor agonists (e.g., semaglutide, tirzepatide) - is the unintended, rapid depletion of lean body mass. Loss of skeletal muscle and bone density exacerbates the risk of sarcopenic obesity, frailty, and premature mortality 323334. Trials utilizing GLP-1 agonists report that an alarming 24% to 40% of the total weight lost can be attributed to lean mass 3234. Research indicates that the combination of abdominal obesity and muscle loss increases the risk of mortality by 83% in adults over age 50 33.
The developers of the fasting mimicking diet assert that the periodic nature of the intervention circumvents chronic muscle catabolism. Data from Longo's cross-over human trials suggest that absolute lean body mass remains largely stable throughout the intermittent fasting cycles, as the body aggressively preserves muscle tissue upon the resumption of a normal, nutrient-dense diet 13. Nevertheless, independent nutritional experts and clinical reviews continuously emphasize the necessity of adequate dietary protein and rigorous resistance training during the 25-day refeeding windows to fully mitigate any potential catabolic effects resulting from the five days of severe hypocaloric intake 1532. Short-term alternate-day fasting models have shown that muscle mass reductions cannot always be attenuated by minor protein supplementation alone, highlighting the critical role of mechanical load (exercise) in preserving lean tissue 1541.
Frailty Syndrome and Vulnerable Populations
The fasting mimicking diet is explicitly contraindicated for individuals experiencing frailty syndrome, severe cognitive impairment, moderate-to-severe functional dependence, or those with a life expectancy of fewer than six months 3536. Frailty represents a state of critically diminished physiological reserve, making vulnerable elderly patients highly susceptible to the hypotensive, hypoglycemic, and catabolic shifts induced by the diet. For older adults exhibiting signs of pre-frailty, ongoing clinical trials in primary care settings prioritize multicomponent interventions involving Mediterranean diets with augmented, rather than restricted, protein intakes, combined with structured resistance exercise to reverse functional decline 3035.
Furthermore, the diet should not be attempted by pregnant or lactating individuals, those with a history of severe eating disorders, or patients with unstable type 1 diabetes without rigorous endocrinological supervision.
Nomenclature Confusion: Fibromuscular Dysplasia (FMD)
A critical point of clinical clarification involves the abbreviation "FMD." Within vascular medicine, FMD refers to Fibromuscular Dysplasia, a rare, idiopathic, non-atherosclerotic disease of the arteries that predominantly affects women and can lead to renal artery stenosis, spontaneous coronary artery dissection, aneurysms, and stroke 373846. Patients suffering from Fibromuscular Dysplasia are managed under entirely different cardiological and vascular protocols, which may include revascularization or antihypertensive therapy 38. The dietary acronym for the Fasting Mimicking Diet shares no relation to this vascular pathology, and healthcare providers must be precise in their documentation to avoid catastrophic clinical confusion.
Distinctions from Preoperative Fasting Guidelines
It is also critical to distinguish therapeutic fasting diets from preoperative fasting protocols. The 2026 American Society of Anesthesiologists (ASA) guidelines for preoperative fasting focus exclusively on reducing gastric volume and elevating gastric pH to prevent pulmonary aspiration during general anesthesia or procedural sedation 4739. ASA protocols dictate the cessation of solid food six to eight hours prior to surgery, while permitting clear liquids up to two hours beforehand 4739. Therapeutic dietary interventions like the fasting mimicking diet are designed for metabolic reprogramming, not surgical preparation. The fasting mimicking diet should be paused well in advance of any surgical procedure to ensure the patient has optimal perioperative nutritional reserves, wound healing capacity, and immune competence 473940.
Future Research Directions
The fasting mimicking diet represents a highly structured, scientifically robust approach to capturing the profound longevity and metabolic benefits of caloric restriction while bypassing the sheer impracticality and inherent risks of chronic starvation. By acutely suppressing nutrient-sensing pathways such as IGF-1 and mTOR, the diet triggers widespread autophagic turnover, cellular recycling, and subsequent stem-cell-driven regeneration upon refeeding. Its clinical efficacy is increasingly documented across diverse domains encompassing the reversal of metabolic syndrome, the mitigation of autoimmune enteropathy, and the chemosensitization of refractory tumors.
However, the field necessitates further large-scale, independent, and long-term randomized controlled trials to firmly establish the diet's durability, safety, and real-world compliance outside the parameters of highly supervised clinical environments. Future research must delineate personalized protocols - optimizing cycle frequency, exact caloric deficits, and macronutrient composition based on distinct genetic, metabolic, and phenotypic profiles - to maximize therapeutic outcomes while definitively safeguarding vulnerable populations against the latent risks of sarcopenia and malnutrition.